If there is one uncomfortable truth about healthcare trends in 2026, it is this: digital transformation is no longer a competitive advantage. It is table stakes. The global digital health market is estimated to grow from US$ 312.3 billion in 2026 to US$ 815.7 billion by 2033, demonstrating a compound annual growth rate (CAGR) of 14.7% during this period. Across the global healthcare sector, leaders are navigating an environment shaped by rising expectations, mounting cost pressure, regulatory shifts, and rapid technological acceleration. The institutions that thrive over the next decade will not be the ones that deploy the most tools. They will be the ones that align strategy, operations, and experience into a cohesive system.
The most important trends in healthcare 2026 are systemic shifts. They redefine how care is delivered, monetized, and experienced. Technology serves as the infrastructure for these changes rather than the end goal.
The healthcare sector outlook: growth under pressure
The current healthcare sector outlook is defined by a paradox. Innovation has never been stronger. At the same time, financial and operational strain has never been more visible.
On the innovation side, breakthroughs in precision medicine and advances in liquid biopsies are changing diagnostic speed. The global pipeline for mRNA vaccines continues to expand. The growth of GLP-1 medications is reshaping metabolic and obesity treatment landscapes worldwide. These clinical milestones provide new pathways for patient health.
However, the healthcare industry is simultaneously dealing with rising inflation. Expanding prescription drug spending and payer complexity create friction. Intensified scrutiny around pharmacy benefit management and ongoing PBM reform discussions add to the administrative burden.
In the U.S., the financial implications of Medicare Advantage expansion and broader policy changes globally create a difficult environment. This sector must innovate and optimize at the same time. Cost discipline is not optional. But cost discipline alone is not enough.
Cost containment: experience is a financial lever
When executives think about cost containment, they often focus on procurement, staffing ratios, or reimbursement optimization. Those levers matter. However, many hidden costs originate in experience design.
Fragmented booking systems increase no-shows. Confusing billing processes increase call center volume. Poorly integrated workflows slow down claims processing and complicate revenue cycle management. Administrative complexity around prior authorization drains staff productivity. When patients struggle to navigate care, operations absorb the burden.
The most forward-thinking organizations now understand that experience redesign is a structural cost strategy. Simplified digital intake reduces administrative load. Transparent billing reduces inbound friction. Intelligent reminders reduce missed appointments. Clear communication reduces repetition and rework. In 2026, operational efficiency and patient experience are no longer separate agendas. They are two sides of the same coin.
The healthcare outlook: convenience is reshaping loyalty
There is another strategic shift that deserves executive attention. Convenience is increasingly stronger than brand. Patients may value reputation, but when forced to choose between similar providers, they often default to the one that is easier to access. Approximately 24% of survey respondents indicate a willingness to switch doctors to ensure access to virtual health options.
The global healthcare outlook shows a steady behavioral migration toward providers that offer frictionless digital interaction. This is particularly visible among digitally fluent populations. As expectations shift, even traditionally offline patient groups begin to demand the same clarity and simplicity.
If booking is faster elsewhere, patients move. If lab results are centralized elsewhere, patients move. If billing is clearer elsewhere, patients move.
Digital maturity compounds over time. Organizations that move early build a structural advantage that becomes difficult to displace.
Mobile as infrastructure, not an add-on
One of the defining 2026 healthcare trends is the repositioning of mobile from a marketing tool to an operational backbone. In many boardrooms, mobile still carries the faint aura of an engagement tool. That framing is outdated. In 2026, mobile is the control center of the patient relationship.

A web portal is visited when needed. A mobile application, once installed, becomes a persistent channel. It allows healthcare organizations to maintain ongoing engagement rather than episodic contact. Mobile ecosystems increasingly unify appointment scheduling, diagnostic results, imaging archives, and medication management. They also integrate with remote patient monitoring and home-based care environments.
This is not a cosmetic transformation. It fundamentally changes how patients interact with the system. Consider medication adherence. When digital reminders integrate with smart devices such as automated pill dispensers, adherence improves. Fewer complications lead to fewer admissions. Preventive nudges reduce downstream costs. Mobile becomes the connective tissue between patient behavior and institutional infrastructure.
It is about making the customer’s life simpler by ensuring that the points of access to services are in the right place, at the right time, in the right context—and that they take into account the context the person is in. - Agata Rączewska, CX Expert
AI and clinical decision support: reducing cognitive burden
Artificial intelligence has moved beyond experimental dashboards. One of the most impactful trends in healthcare 2026 is the operationalization of AI-driven clinical decision support. Modern systems can interpret lab values in context, identify longitudinal risk patterns, and surface early warning indicators.

In oncology, AI assists with the interpretation of complex diagnostic data. In chronic disease management, it can flag subtle deterioration before it becomes acute. AI is not replacing clinicians. It is reducing cognitive load. In a system where information volume grows exponentially, interpretation speed becomes a strategic asset. When AI assists in contextualizing patient data, clinicians gain time and clarity. Over time, this will influence not only outcomes but also workforce sustainability.
Preventive care, longevity, and ageing in place
Another unmistakable shift in the healthcare sector is the movement toward prevention and longevity. The traditional model of care has been reactive. Symptoms trigger visits. Visits trigger treatment. Treatment concludes the interaction.
The emerging model is continuous. Digital tracking, structured reminders, and integrated analytics enable proactive intervention. This aligns directly with global trends around longevity and healthy lifespan extension. The rise of ageing in place strategies illustrates this well. Patients increasingly want to remain independent longer. They are supported by connected monitoring tools rather than institutional care.
Integrated virtual care platforms and wearable data streams enable this transition. The ability to monitor health remotely while maintaining centralized data continuity strengthens both patient satisfaction and cost efficiency. Preventive ecosystems also improve chronic disease management. Sustained engagement is more valuable than isolated appointments in these cases.
Specialty growth and structural integration
High-growth specialty areas are also reshaping the broader healthcare sector. The expansion of ambulatory surgery centers reflects a shift toward outpatient efficiency. Oncology continues to evolve rapidly through cancer diagnostics innovation and advanced therapeutic approaches.
Meanwhile, the management of metabolic conditions through therapies such as GLP-1 receptor agonists has introduced both opportunity and reimbursement complexity. The financial strain tied to new drug categories reinforces the importance of integrated care pathways and data visibility. These developments require digital coordination. Fragmented data silos cannot support complex, multidisciplinary care at scale.
Financial complexity and policy evolution
Healthcare systems operate within dense regulatory frameworks. Ongoing healthcare policy changes influence reimbursement, pricing transparency, and reporting obligations. In the U.S., shifts in Medicare Advantage enrollment and scrutiny around pharmacy benefit management structures are altering revenue models.
Globally, governments are placing increased pressure on affordability and accountability. Digital infrastructure becomes a strategic asset in navigating this environment. Adaptable systems allow organizations to respond quickly to regulatory adjustments and payer demands.
Health equity and digital responsibility
As healthcare digitizes, leaders must address health equity intentionally. Accessibility cannot be an afterthought. Inclusive digital design, multilingual support, and clear consent flows are necessary components of a modern system. They influence adoption rates and trust.
Simultaneously, the risk of healthcare data breaches grows as systems become more interconnected. The average cost of a healthcare data breach reached $7.42 million in 2026. Cybersecurity investment must scale with digital ambition. Trust is expensive to rebuild once it is lost. In many ways, trust becomes a competitive currency. Patients are increasingly aware of their rights and data vulnerabilities. Organizations that protect patient data rigorously will earn loyalty. Those that do not will pay in reputation and market share.
Experience as a strategic discipline
Experiential excellence is no longer a design ideal. It is an operational imperative. Too often, organizations treat digital health services as tactical products rather than strategic platforms. They build portals, apps, or chatbots in isolation. They fail to align them with clinical workflows, revenue goals, or patient psychology.
This leads to fragmentation. It results in great tools that do not integrate with booking systems, payment engines, or clinician workflows. Patients adopt these tools briefly and then abandon them. The most forward-thinking organizations embed experience as a mindset that guides decision-making at every level. This means:
- Careful attention to UX writing, not only UI design
- Strategic integration of patient feedback loops
- Measurement of longitudinal engagement metrics rather than just NPS
- Early involvement of marketing, sales, and clinical leadership
Experience must be operationalized. It cannot simply be idealized.
Miquido’s role: turning strategic ambition into tactical delivery
One of the clearest examples of experience-driven transformation can be found in real-world healthcare app development. Miquido’s engagement with healthcare digital platforms illustrates how strategic intent turns into real patient impact.
A notable example is the Diagnostyka 2.0 mobile platform. This platform was rebuilt in Flutter to unify diagnostics across patient workflows. The goal was to redesign how patients interact with lab data, appointments, and results from a single mobile hub. Flutter’s cross-platform architecture allowed the team to deliver consistent experiences on both iOS and Android. It maintained high performance and a native feel.
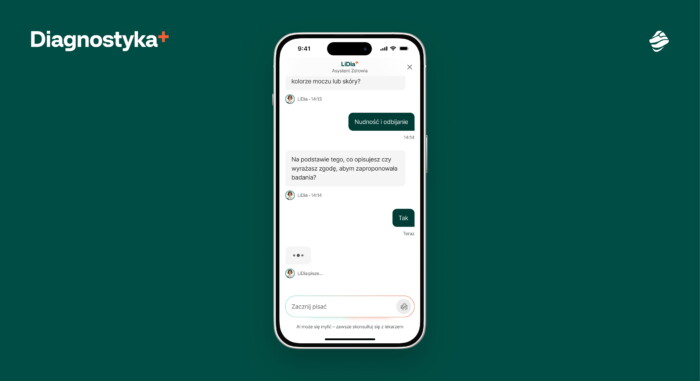
For patients, this meant:
- Immediate access to historical lab results
- Seamless appointment scheduling
- Intuitive navigation across complex medical data
- Real-time notifications and reminders
It showed how a thoughtful digital platform can increase both operational efficiency and patient satisfaction. The Diagnostyka example is not an isolated case. It reflects a broader pattern. When healthcare technology is developed as infrastructure, it drives measurable outcomes across clinical, operational, and financial dimensions.
Healthcare is for everyone. Everyone should have the same right and the same ease of access to their results and health information. - Bogusław Podhalicz, UX Design Lead at Miquido
The risk of inaction
What happens to organizations that fail to accelerate? They may not disappear overnight. The healthcare market still supports traditional models in many regions. However, stagnation compounds. As digital leaders improve retention and streamline operations, laggards lose share gradually.
Younger demographics prioritize seamless digital access. As this population ages, digital preference becomes universal. When price and proximity are similar, convenience wins. Over time, this effect becomes cumulative. Digital maturity becomes a moat.
The strategic imperative for 2026
The defining message behind healthcare trends 2026 is not about technology alone. It is about redesigning the system around clarity, continuity, and intelligence.
Winning organizations will:
- Embed digital infrastructure at the core
- Use AI to augment decision-making
- Integrate preventive and chronic care pathways
- Treat cost containment as a design challenge
- Align innovation with regulatory realities
- Protect patient data as a strategic asset
- Prioritize patient-centered simplicity across all touchpoints
The global healthcare sector outlook suggests that the next decade will reward those who eliminate friction. For C-level leaders, the strategic choice is straightforward. You can digitize legacy systems and preserve existing complexity. Or you can redesign the system around the patient and build a structurally stronger organization for the future. 2026 will make that difference visible.

![[header] healthcare trends 2026 – a patient centric future](https://www.miquido.com/wp-content/uploads/2023/12/header-healthcare-trends-2026-–-a-patient-centric-future-1920x1280.jpg)



![[header] 6 mobile app development mistakes to avoid](https://www.miquido.com/wp-content/uploads/2021/12/header-6-mobile-app-development-mistakes-to-avoid-432x288.jpg)