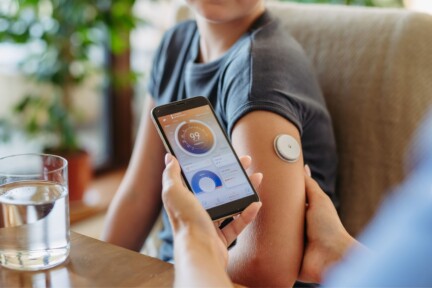
In 2021, the global healthcare sector faced a critical challenge: providing care with minimal physical contact. Remote solutions solved the immediate problem, but they exposed a deeper flaw – our systems simply do not connect the dots.
As we move through 2026, the mantra for healthcare founders building monitoring apps, diagnostics, or clinic management tools is no longer just "digitalization," but true interoperability. In practice, however, many healthcare systems are outdated, and their architecture does not allow for effective, seamless integration. As a result, data gets stuck between them; systems fail to communicate properly, preventing the activation of crucial alerts or triggers related to diagnostics or missing documentation.
How to develop custom healthcare software? Tips to keep your medical software solution safe, flexible and future-proof
To make Healthcare 4.0 a reality, we must build and rebuild with these challenges in mind, preventing these silos from forming in the first place. Whether you are looking for healthcare software development services or starting a new venture, the following guide outlines how to navigate the technical and clinical landscape of 2026.

1. Adopt a modular, integration-first architecture to scale beyond "point solutions"
Modern healthcare is moving away from isolated apps. McKinsey's analysis of the evolution of artificial intelligence in healthcare concludes that the sector is moving from fragile point solutions toward modular systems powered by domain models, intelligent agents, and robust data governance. As a part of this shift, the modular architecture becomes the foundation for scalable, sustainable healthcare innovation.
However, founders face a structural bottleneck. A PMC-published study on deploying digital health tools identifies integration with existing infrastructure as a primary barrier, noting that internal departments often lack bandwidth to validate and maintain external integrations – a gap that legal and compliance teams exploit to block adoption.
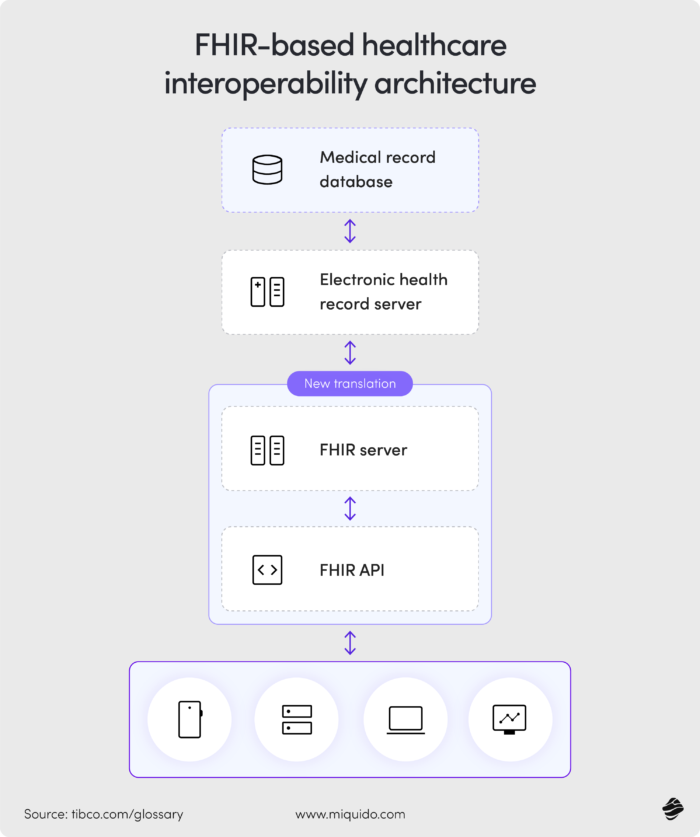
Healthcare software development that makes data match
How to avoid it when building custom medical software? One of the things you can do is to break the "hierarchical wall" with FHIR-native storage. Legacy systems like Epic often use MUMPS (a hierarchical database), while modern apps use SQL or NoSQL. This "impedance mismatch" often causes integrations to time out.
To avoid this issue, build your 2026 stack using FHIR-Native Storage. Think of it as a universal shipping container for data; because every piece of information is packed in the same standardized format from the moment it is created, it can be instantly recognized and used by any other modern system without tedious translation. Don't just "wrap" your data in FHIR; store it as FHIR resources (Resource-Oriented Architecture). This approach ensures that your electronic health records remain fluid and accessible across the entire ecosystem without requiring custom middleware for every new connection.
Adopt the "Lego" approach: Instead of building a giant, rigid table of data, treat every piece of information (a heart rate, a lab result) as a separate "Lego brick" that can be moved individually without breaking the whole house.
2. Implement edge layers to manage wearable data velocity without system crashes
Currently, wearables are still largely tied to the wellness industry rather than healthcare, supporting individual fitness and health monitoring. This, however, is about to change. For many people, especially those affected by chronic diseases, integrating wearables with healthcare software applications – for example, clinic apps, patient accounts, or hospital systems – could significantly facilitate treatment and prevention.
Take a person with diabetes, for example: a continuous glucose monitor could stream real-time sugar levels directly to a clinical decision support system, allowing for proactive insulin adjustments before a crisis occurs.
Similarly, for patients with heart disease, a wearable could detect early signs of arrhythmia and alert a specialist before the patient even feels a symptom. Wherever measurable parameters matter for a diagnosis and quick reaction is a matter of life or death, this type of innovation can truly make a difference.
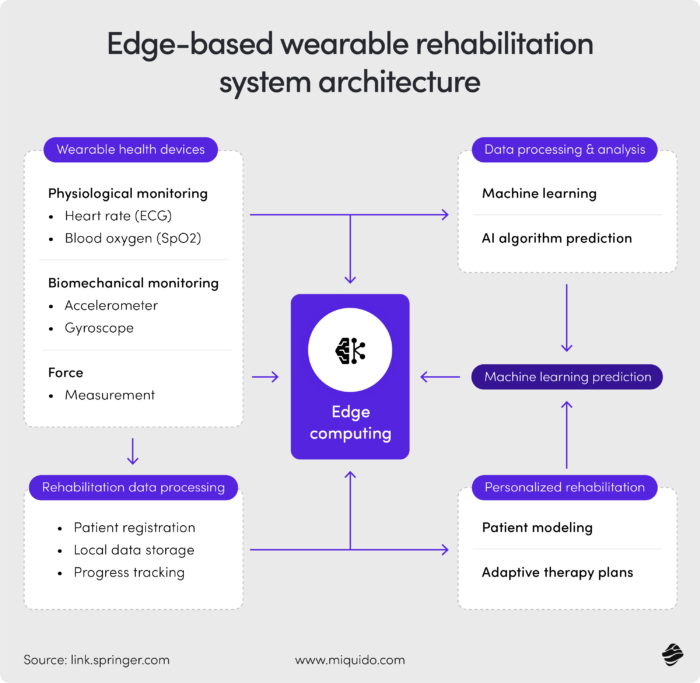
For this vision of the future to work efficiently instead of unnecessarily overloading the system, it is necessary to consider technical aspects when creating medical software development projects. Wearables generate high-frequency streams (100+ data points/hour), but transactional EHRs are designed for point-in-time entries (1 result/day). IntechOpen research highlights that direct streaming into an EHR causes "I/O locks" (system freezes) and "alert fatigue," where clinicians ignore 90% of notifications.
To manage this gap, your healthcare software solution can use Complex Event Processing (CEP) at the edge. Essentially, you create a "buffer zone" (Stream Decoupling) where your app analyzes data before it touches the hospital system. This way, it only promotes data to the medical record when it meets clinical significance (e.g., $HR > 150$ for 5 minutes).
Such adaptation makes a significant difference, translating to better usability of remote patient monitoring systems. A Springer Nature peer-reviewed study on AI-powered edge computing for wearable ECG monitoring demonstrated that AI-driven alert filtering at the edge reduced false alarms by 35%, directly validating clinical efficiency gains.
3. Implement on-device computing instead of sending data to the cloud
A few years ago, the trend in software development in healthcare was to send everything to the cloud. In 2026, the intelligence is shifting back to the device itself, particularly utilizing modern browser capabilities like Chrome's local processing.
On-device computing offers several key advantages:
- Performance: It accelerates the entire process by eliminating latency, leading to increased user satisfaction.
- Privacy: It provides significantly greater data privacy. This is crucial in the healthcare industry, where any data breach can have massive reputational and legal consequences. By keeping data local, you simplify the path to creating HIPAA compliant software.
The challenges include managing fragmented hardware capabilities, but for healthcare app development, the trade-off is worth it: users get real-time feedback, and providers reduce their liability for data in transit.
4. Move beyond PDFs to semantic interoperability for automated rescue triggers
You probably know this from experience: test results arrive as PDFs and get lost between emails. The fact that this is problematic from a user experience standpoint is only one side of the coin – we describe the potential consequences and solutions in our article on how to improve patient experience. However, it is also a nightmare for logistics and data processing for various life-saving automations.
Diagnostic centers often provide "seamless access" via a PDF. But to a computer, a PDF is just a picture; it cannot trigger an automated rescue alert. As seen in the NHS QRISK2 failure, if the coding between dwoma systems doesn't match perfectly, risk scores are calculated incorrectly, leading to years of medical errors.
One of the ways to avoid it is to mandate semantic terminology servers. In practice, this means your software uses a centralized "translator" that maps every local medical term to a globally recognized code.
Without diving into deeply technical aspects, you should implement a system where clinical data is validated against standard dictionaries in real-time. Never allow "free text" for clinical values. Instead, use binding to ValueSets (SNOMED-CT / LOINC). This ensures that when your app says “penicillin allergy," every other system understands exactly what that means.
Securing this seamless “understanding” is essential in custom healthcare software development, as it prevents clinical errors that can be fatal. According to a peer-reviewed PubMed study, incorrect principal diagnosis selection accounted for 13% of DRG changes and missing additional codes for 29%, with poor documentation quality being the single most significant driver of coding error.
5. Bridge the Public-Private divide using standardized EU frameworks
Systemic problems resulting from staff shortages, underfunding of healthcare sectors, and the closing of facilities are difficult to solve with software alone – it is more a matter of resources. However, facilitating connections between the public and private sectors can be a major pillar of healthcare development in 2026.
In many EU countries, the public sector redirects patients to private clinics for tests. A PMC-published study on Public-Private Partnerships (PPPs) identifies these collaborative models as the primary mechanism for overcoming institutional shortcomings. However, the patient must navigate the registration and documentation transfer. This process is prone to errors and delays, but also high churn. The proof is in the data: Forrester's Q2 2024 report found that healthcare organizations are losing patients to access friction – repeated handoffs and fragmented data. It is also a sensitive area for data processing legislation, requiring rigorous consent management.
EHDS-ready healthcare software solution
An important tip for software intended for the European market is to align with the European Health Data Space (EHDS). Currently, the framework is just starting to take effect, but it is worth keeping in mind when designing systems that data interoperability is something the EU will strive for and require within the next few years. It is also a significant financial milestone: The EHDS framework is expected to generate €11 billion in savings over the next decade and drive a 20-30% expansion in the digital health sector.
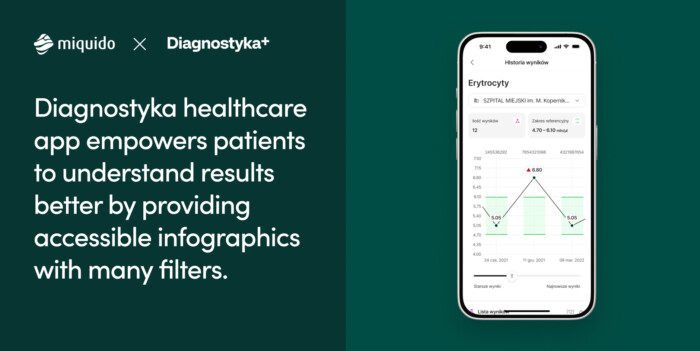
At the moment, in many countries, secure authorization, document transfer, and data exchange between public and private providers are streamlined with the help of government profiles. In Poland, for example, healthcare software development services are increasingly utilizing authentication through IKP (Internetowe Konto Pacjenta) in the gov app. Through these portals, authorizing a specific facility is a matter of a few clicks. This was the solution chosen by a diagnostic network we collaborated with to create the Diagnostyka 2.0 application, revolutionizing the patient service approach in this niche.
6. Prioritize "empathy-driven simplicity" to combat cognitive fatigue and burnout
Healthcare software must evolve beyond functional UI. A peer-reviewed PMC study confirms that Human-Centered Design (HCD) is essential for ensuring technology addresses real patient pain points.
While we have healthcare solutions available, they are often not made for the patients. Athenahealth's 2025 research found that while 86% of patients have used a portal, the median Patient Digital Engagement Index is only ~14 out of 100, revealing a massive gap between intent and frictionless engagement.
On top of that, the inappropriately designed tools can also propel the physician burnout crisis. We have already mentioned the numerous technical challenges of legacy healthcare systems. But their design is also problematic, negatively affecting the efficiency of healthcare teams. Physicians gave EHRs a SUS score of 45.9 – a grade of 'F'. Research in JAMIA found that 86.9% of primary care physicians reported excessive alert burden.
Healthcare software systems that support everyday work
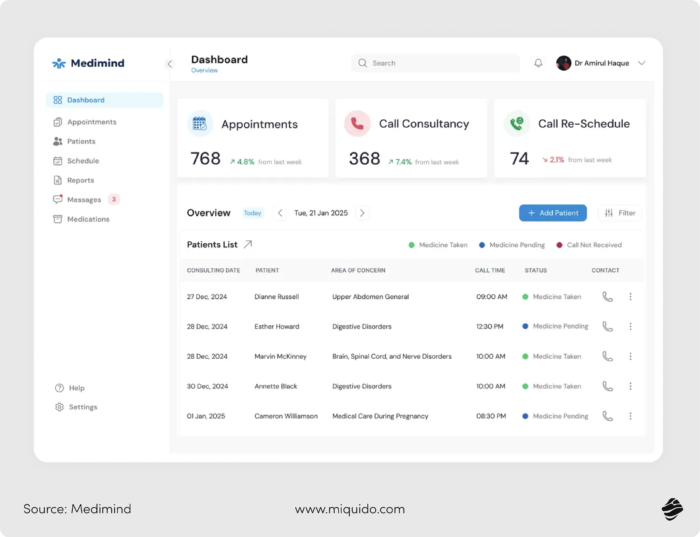
How to build custom healthcare software that actually makes practitioners' jobs easier? The answer, of course, is: it depends – on their specialty and the problems they face daily. One thing is certain – the average healthcare professional does not need fancy features, but rather tools that actually relieve them in their daily work. This system overload is the biggest problem, and every minute unlocked by technology is worth its weight in gold.
What could make a difference? Building intelligent filtering systems. For example, if the system floods staff with alerts, detection rates might go up on paper, but in reality, the team is cognitively overloaded and unable to process them effectively. You need to go a step further and build an effective filtering system – based on actual, verified medical input and not just an LLM’s output – to prioritize what is truly critical.
6. Maximize revenue by treating "speed-to-diagnosis" as a financial lever
Strategic software should replicate fast-track clinical models. A study in npj Digital Medicine found that digital-first pathways were associated with 23% lower costs without increasing follow-up visits. Conversely, World Economic Forum (2026) reports that diagnostic delays for rare conditions cost up to $517,000 per patient. By investing in population health management tools that identify risks early, providers can drastically reduce long-term costs.
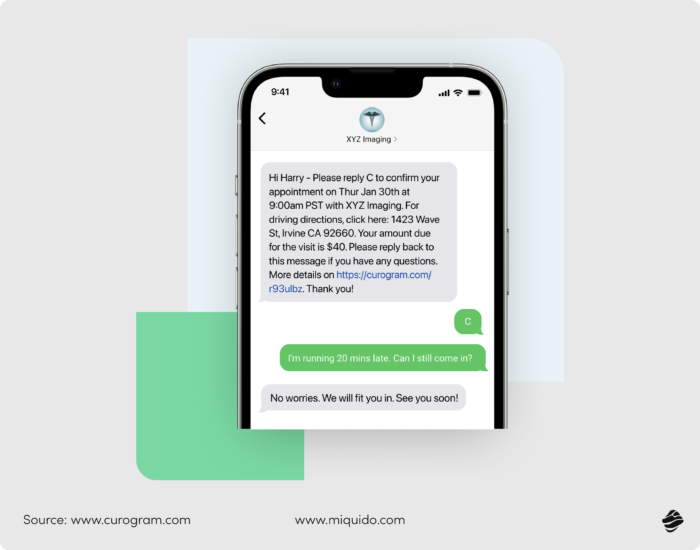
What could make a difference? Automating proactive scheduling to eliminate no-shows. Patient no-shows cost the U.S. system $150 billion annually, with an average cost per missed appointment of $196 (PMC).
The ROI of communication is clear. The patient should receive at least several reminders with a full set of information (depending on the nature of the visit – date, time, location, room, requirements regarding preparation for the procedure). Otherwise, automations can only frustrate, creating a sense in the patient that they are being cut off by a "digital wall" from the person responsible for their treatment.
By implementing such Memorial Hospital at Gulfport achieved a 28% reduction in no-shows, generating over $1 million annually. This is critical because patients who miss just one appointment have an attrition rate of 70% (Artera).
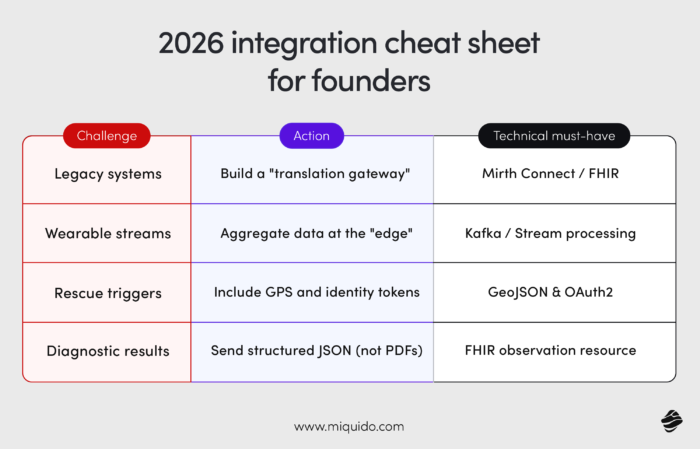
Strategic roadmap for medical software development and innovation
The future of medical software development in 2026 demands a shift from isolated tools to interconnected ecosystems that prioritize the patient journey. Successful healthcare development now relies on the ability to merge real-time monitoring with historical records while maintaining absolute system stability. By focusing on these integration-first principles, founders can transform modern clinical challenges into scalable digital opportunities.
Investing in custom software development for healthcare allows organizations to bypass the limitations of legacy infrastructure and build modular, future-proof platforms. These solutions must leverage advanced healthcare data analytics to provide actionable insights that reduce clinician burnout and improve diagnostic speed. When data flows seamlessly and intelligently, the entire healthcare delivery model becomes more efficient and cost-effective.
Finally, the convergence of medical device software and robust healthcare cybersecurity remains the ultimate safeguard for patient trust and safety. Every wearable sensor and diagnostic tool must be protected by rigorous encryption standards to prevent high-stakes data breaches. Prioritizing these security protocols ensures that your innovation not only meets regulatory compliance but also delivers reliable, life-saving care.

![[header] how to develop healthcare software in 2026 a blueprint for founders, clinics, and diagnostic innovators (1)](https://www.miquido.com/wp-content/uploads/2026/04/header-how-to-develop-healthcare-software-in-2026_-a-blueprint-for-founders-clinics-and-diagnostic-innovators-1-1920x1280.jpg)


![[header] how to develop healthcare software in 2026 a blueprint for founders, clinics, and diagnostic innovators (1)](https://www.miquido.com/wp-content/uploads/2026/04/header-how-to-develop-healthcare-software-in-2026_-a-blueprint-for-founders-clinics-and-diagnostic-innovators-1-432x288.jpg)