It’s hard to remember a time when healthcare wasn’t overwhelmed. Technology was supposed to change that. And the radical change has taken place, indeed.
Technological advancements now allow us to perform surgeries that were impossible until recently, supporting surgeons in their titanic efforts. Thanks to AI, which is already deeply embedded in the clinical path, we can analyze X-rays, MRIs, and CT scans incomparably faster and with greater accuracy. We even grow tissues for transplantation in labs, simulate disease progression on digital twins, and create personalized vaccines.
We also placed immense hope in AI to radically transform diagnostics and the patient journey. And while a lot has improved, the patient in 2026 still faces difficulties that properly designed and implemented mobile health apps could solve once and for all. The key is a customer experience (CX) approach, where the client's pain points are the central axis of development.
In today's article, together with a CX expert from Miquido, we break this issue down into its core components and look for market gaps you can fill, contributing to a better patient experience.

Positive patient experience is healthcare industry’s blindspot
While medical costs worldwide are projected to rise by 10.3% in 2026, the most significant waste isn't in the medicine itself. It’s in the friction of the journey.
The processes and tools available to patients often fail to help them avoid frustration – and in fact, they often add to it. This frequently extends the overall treatment path and limits its effectiveness: the patient gets lost in the system, disappears, and only returns when their condition worsens, which prolongs treatment and lowers the prognosis. This is especially significant in public healthcare, where, in financially strained realities, it is crucial to serve the patient as quickly as possible.
"It pays off for the hospital to cure us faster. If a patient is cured in two weeks because the system was streamlined, they don't return as a cost. Good CX is also an ultimate cost-optimization strategy."
Agata Rączewska, CX Specialist at Miquido
To enhance patient experience, it’s not enough to implement new, shiny features. Good CX goes much deeper, allowing for an understanding of customer needs and filtering the app's logic, functions, interface, conveniences, processes, and internal mechanisms through them.
As the Miquido specialist emphasizes, CX specialists are not just experts at placing boxes on a screen because they know where they "should" be; they are experts at connecting the needs of your clients and your business with those boxes. Only then do they make sense on the screen. This is particularly important in healthcare, where customer-centric approach is not only the matter of user satisfaction, but of wellbeing and the improvement of health.
Solving the "blank slate" problem: Improving healthcare for the modern patient
The most profound pain point in both public and private systems is the "anonymity tax." Every time a patient meets a new specialist, they are forced to restart their narrative from zero.
In many countries, the issue of transferring documentation is handled by IT processes, allowing private and public facilities to exchange patient documents despite tight legal and GDPR restrictions. Take Poland, for example, where every patient has access to the Internet Patient Account (IKP). Through it, they can quickly and conveniently authorize facilities or specific medics to access their documents.

In theory, this should solve the problem – the doctor has access to the test registry and all available documents. But in practice, it’s not like that at all. Doctors are overworked and heavily booked; they don't have time to familiarize themselves with individual PDFs before each visit, let alone deeply track the progress of treatment over time.
The missing "big picture": Crucial pain point on a road to improving patient care
As a result, data stays siloed. Patients feel like strangers at every appointment. Part of the visit is spent summarizing medical history and conducting an in-depth interview. It happens that constant rescheduling and delays force patients to take leave from work or travel hours, only to find the provider lacks their full history.
But the problem isn't just the emotional layer. A lack of interdisciplinary communication leads to treatment failure. Example: A patient’s dental health might be the hidden trigger for an autoimmune skin flare-up, but because the dentist and the dermatologist never "connect the dots," the patient continues their treatment without seeing any results.

The CX opportunity: Path-based ownership
It could look different – and it’s within reach with generative tools and good designers on board. Having already established appropriate data processing processes, one could create a Smart Treatment Map that follows the patient, not the provider.
Instead of a list of PDFs, such a map is a living timeline where the system flags cross-specialty correlations automatically. It serves both the patient and healthcare professionals, helping both sides see the "big picture." It immediately flags missing tests or check-ups, helping the doctor direct the visit and making it easier for the patient to take matters into their own hands.

If national or regional systems like IKP exist, such a map could be integrated with them. Alternatively, it could be available within an app.
When the system "knows" the patient, the risk of misdiagnosis and redundant testing – two of the highest costs in healthcare – drops significantly.
Diagnostics and information stress: Enhancing patient experience through visualization
If you’ve ever had the chance to receive test results you’ve been waiting for a long time, you surely remember how stressful that experience can be. Even more so because you usually don't get the result "on a silver platter" – you have to wade through a thicket of tables and numbers.
Receiving results is a moment of peak psychological stress. Currently, most diagnostic providers fail the patient at the exact moment they are most vulnerable by delivering a “data wall”.
Cognitive fatigue and lack of context: Main obstacles to positive patient experience in diagnostics
Opening a portal to see a wall of medical jargon and bolded numbers without explanation creates cognitive fatigue. This can lead not only to unnecessary stress but also to misunderstanding and the exaggeration or, conversely, the trivialization of one's health status.
Another major problem is the fragmentation of results. Individual tests often say little about health – only looking at them in perspective provides the desired context. In certain situations, a single result is meaningless without the "direction of travel." An example: doctors judge a pregnant woman's weight as a change over time. Healthcare CX needs to apply this to all data – showing a 5-year trend to prove treatment efficacy.

The CX opportunity: Longitudinal visualization
To be fully useful, results must be visualized as a story. The user should not have to pore over numbers and compare them manually; instead, they should be translated into accessible visualizations that show progress and allow filtering by time periods and specific parameters.
This "story" would take the form of an interactive health timeline where color-coded markers indicate status changes and AI-driven insights explain what fluctuations mean for the user’s long-term goals. Key features would include a "Compare with baseline" toggle and a one-click summary generation that prepares a simplified visual report for the next doctor's appointment.
Founders who build tools that "translate" raw data into visual trends will win the loyalty of patients who currently feel abandoned by their own test results.

Case Study: Diagnostyka – Redefining results through AI and UX
Diagnostyka, the leader in laboratory diagnostics in Poland, is a prime example of a founder-mindset company that transformed a "data wall" into a patient-centric experience. In collaboration with Miquido, they rebuilt their mobile app to move beyond transactional test-checking and toward long-term health management. The project focused on creating a secure, intuitive architecture that integrates seamlessly with existing medical systems while simplifying the user's journey.
To solve the issue of data fragmentation and stress, the app introduced innovative tools like LiDia, an AI assistant, and the Profilaktometr. LiDia acts as a conversational guide that helps patients understand which tests they need based on verified medical knowledge, while the Profilaktometr uses gamification to visualize the completion of recommended check-ups. These features turn raw, intimidating data into a manageable and engaging health habit.
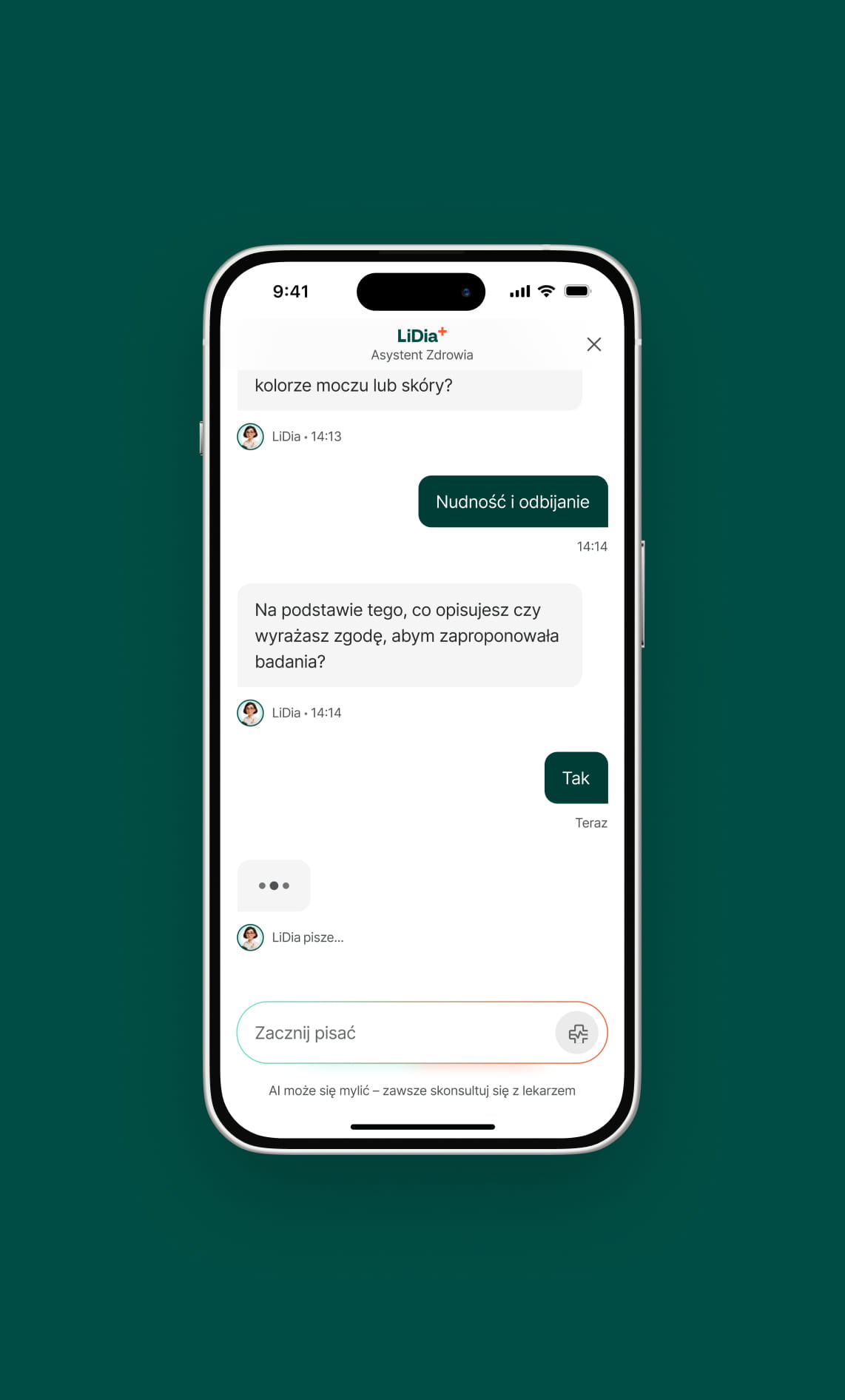
The results of this CX-driven approach are clear: the app saw a 360% growth in its user base and now supports 138,000 active users. By prioritizing accessibility and clear visualizations, Diagnostyka has set a new benchmark in the European MedTech market. The platform demonstrates that when medical data is presented with context and clarity, it empowers patients rather than overwhelming them.
The onboarding labirynt: Improving patient experience for global citizens
In an era of unprecedented global mobility, healthcare systems remain stubbornly parochial. Navigating a local medical landscape – with its unique bureaucratic quirks and "secret" unwritten guidelines – has become a major barrier for expats, digital nomads, and refugees alike.
Wall of exclusion barring patients from access
The "onboarding" process into a new country’s healthcare system is often a minefield of unclear guidelines. Patients frequently encounter niche requirements for local ID numbers that don't exist in their home countries, conflicting information on necessary documentation, and hidden fees that only surface at the point of care. For instance: Polish
Furthermore, many systems still rely on a "phone-first" culture. The requirement for voice contact in a local language creates a literal wall of exclusion for non-natives, leading to delayed treatments and high levels of patient anxiety.
The CX opportunity: Systemic guidelines & AI triage
The gap here isn't just linguistic, but systemic. There is a massive opportunity for AI-driven "System Guides" that go beyond simple translation, improving the patient experience.
Imagine a platform that doesn't just translate words, but translates the process. It acts as a digital concierge, telling a patient exactly which document they need for their specific residency status and why, while offering asynchronous, text-based triage.
This reduces the administrative burden on providers by ensuring patients arrive with the correct "paperwork" (digital or otherwise) and have already been screened for urgency.
Silver economy: A market gap to improve patient satisfaction
Current HealthTech trends exhibit a massive bias toward Millennials and Gen Z, yet the demographic that consumes the most healthcare – the aging population – is frequently met with the most hostile CX.
While younger users can easily "let go" of old design patterns and adapt to radical changes, older users have more deeply ingrained habits. For them, a sudden overhaul of navigation might be much more than just a minor inconvenience, becoming a barrier to care.
"Parenthood" burden and exclusion by design
The failure of senior-centric UX creates a "parenthood" burden: complex, fragmented interfaces often force adult children to manage their parents' entire treatment plans, leading to burnout for the caregiver and a loss of autonomy for the patient. Many high-tech portals suffer from exclusion by design, assuming a level of digital literacy, high-contrast vision, and fine motor skills that actively alienate seniors.
In just the last decade, we’ve seen milestone shifts in interface design: feed-first apps have replaced menu-first ones, and modal flows have taken over for full-page transitions. Now, we are on the verge of another shift driven by our interactions with LLMs. While a true "Zero-UI" era may still be on the horizon, interfaces are moving in that direction. We must ask ourselves: are we leaving seniors behind in this evolution? When a healthcare app requires tiny toggle switches or complex multi-factor authentication that times out too quickly, it isn't just a "bad UI" but a clinical barrier.
The CX opportunity: Adaptive accessibility
This is arguably the most underserved market in healthcare today. As the "Silver Economy" grows, the demand for accessible technology will skyrocket. However, accessibility isn't just about the elderly; it’s about digital wellbeing across the board. For Generation Z and below, this means prioritizing alerts so they aren't overwhelmed by "notification fatigue," while for seniors, it means ensuring they don't lose the thread of their medical journey due to over-complicated layouts.
A potential solution lies in giving the user agency over their interface. While it requires more effort during the design phase, providing various UI models – such as a choice between a traditional menu or a modern feed, and customizable font and icon sizes – makes the patient feel truly cared for.
Proactive safety: Healthcare patient experience in critical conditions
In states of potential danger, waiting for a callback is more than a frustration – it is a failure of care. While we celebrate the era of "connected health," the current patient experience remains dangerously reactive. The next generation of CX must move beyond passive monitoring and integrate medical devices directly into the response loop.
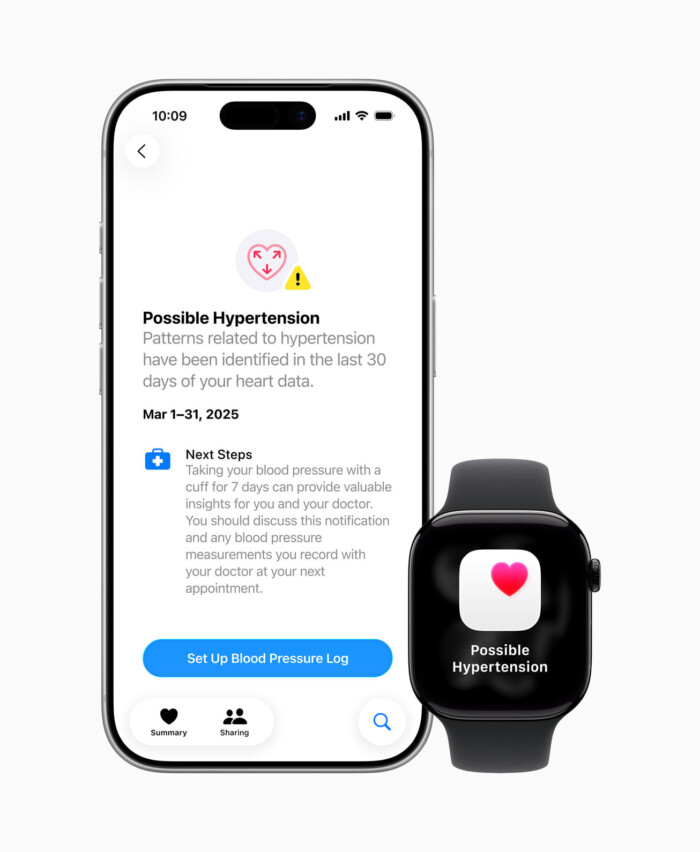
Passive waiting and isolated data are obstacles to improving healthcare outcomes
Currently, patients managing high-risk conditions, such as cardiac issues or brittle diabetes, often find themselves trapped in the same administrative bottlenecks as those with minor ailments. They wait in the same phone queues and navigate the same generic booking portals.
Furthermore, we face a massive data isolation problem: the life-saving information from wearable BP monitors or heart rate sensors rarely triggers an automatic clinic response. The data exists in the cloud, but the "action" remains manual, leaving the burden of crisis detection entirely on the patient.
The CX opportunity: Automated fast-tracks
The shift from "monitoring" to "intervention" is where the most significant medical outcomes are hidden. By breaking down the silos between hardware and clinical workflows, we can create a system that acts before the patient even realizes they are in trouble.
Seamless integration with medical devices to send automatic alerts and personalized recommendations. If a patient’s parameters hit a predefined "danger zone," the system shouldn't just send a notification – it should trigger a "Fast Track" appointment, automatically bypassing standard scheduling and alerting the medical team. This is CX as a safety net: moving from a system that records illness to one that actively preserves safety.
Pharmacy revolution: Reliability to increase patient satisfaction
The pharmacy is perhaps the most frequent touchpoint in the entire healthcare journey, yet it remains one of the most reactive and frustrating. It is the "last mile" of care, and currently, that mile is full of hurdles that undermine treatment efficacy and patient trust.
The "wait-and-see" Model: an obstacle to better patient experience last-mile
We are still operating on a legacy "Wait-and-See" model. Patients – often those who are feeling at their worst – travel to physical pharmacies only to find that their specific medication is out of stock.
This creates an ownership void: the responsibility for planning medication supplies and hunting down inventory rests entirely on the sick patient. In a world of 15-minute grocery deliveries, the fact that a patient has to visit three different locations to find a life-saving antibiotic is a glaring CX failure.
The CX opportunity: Proactive inventory management
There is a massive market gap for a pharmacy concierge model that treats medication as a critical service rather than a simple retail transaction. By connecting e-prescriptions directly with real-time stock management and patient calendars, the pharmacy can become a proactive partner in the healing process.
"There is huge potential here. Pharmacies should call the patient: 'Your specific medication arrives Tuesday; we have reserved it for you. Would you like to pick it up at 4 PM?'"
Agata Rączewska, CX Specialist at Miquido
This level of proactive communication removes the cognitive load from the patient. When the system takes ownership of the supply chain, "out of stock" ceases to be the patient's problem and becomes a logistics task handled behind the scenes.
Modern solutions: 24/7 access and self-service for better healthcare experiences
The traditional "call back during office hours" model is a relic of the past. Modern care requires moving beyond restricted phone lines to a multi-channel ecosystem (chat, video, AI triage) that provides 24/7 security.
By implementing AI-driven triage, systems can provide instant guidance without overburdening human staff, ensuring that a patient’s anxiety is addressed at 3 AM just as effectively as at 3 PM. This accessibility is one of the most direct ways to increase patient satisfaction with artificial intelligence in healthcare, as it replaces uncertainty with immediate, actionable steps.
Self-service scheduling: Returning agency to the patient
True "Path-Based Ownership" starts with the patient having full control over their calendar. Self-service scheduling and management should be the default, allowing users to book, reschedule, or cancel appointments in seconds without a single phone call.
Missed appointments cost the NHS nearly £1 billion annually. When a system makes it difficult to reschedule or provides no proactive reminders, it effectively subsidizes its own inefficiency.
Reducing this "no-show" rate through better self-service and proactive notifications is a critical financial strategy to improve the patient experience while protecting the provider's resources. While it can increase patient satisfaction in hospitals, it also
Conclusion: CX as the new clinical standard
The innovations we’ve discussed – from smart treatment maps to proactive pharmacy concierges –represent a shift in how we view the patient. They are no longer just a "case" to be handled, but a client to be supported through a high-stress journey.
By closing these market gaps, healthcare providers can transform the "friction of the journey" into a streamlined, dignified, and ultimately more effective path to recovery.

Many creative ways to increase patient satisfaction in hospitals are yet to be implemented and could become a breakthrough in a modern approach to customer experience in healthcare. With our expertise in healthcare industry, we can help you innovate and bring them to life.


![[header] how technology can improve patient experience a practical guide for healthcare providers](https://www.miquido.com/wp-content/uploads/2026/03/header-how-technology-can-improve-patient-experience_-a-practical-guide-for-healthcare-providers-1920x1280.jpg)

![[header] how technology can improve patient experience a practical guide for healthcare providers](https://www.miquido.com/wp-content/uploads/2026/03/header-how-technology-can-improve-patient-experience_-a-practical-guide-for-healthcare-providers-432x288.jpg)


![[header] customer experience in healthcare when technology finally learns to care](https://www.miquido.com/wp-content/uploads/2026/02/header-customer-experience-in-healthcare_-when-technology-finally-learns-to-care-432x288.jpg)