In modern medicine, the focus remains primarily on the "what"—the specific diagnosis, the prescribed drug, or the necessary surgery. However, the patient's context is just as critical. True personalization of healthcare addresses the reality that a patient is a person under immense cognitive and emotional stress.
Moving away from a one-size-fits-all model requires more than just better medicine. It requires a highly tailored, patient-centered approach that accounts for the environment in which care is delivered. This shift is not merely a technological upgrade. It represents a fundamental change in the philosophy of healthcare delivery.
Defining personalized healthcare in 2026
Personalized healthcare is a medical model that categorizes patients into specific groups to tailor interventions. Decisions and products are customized for the individual based on their predicted response or risk of disease. To implement this effectively, healthcare organizations must look beyond biological markers alone.
A comprehensive personalization strategy includes clinical data such as genomics and genetic profiles. It also incorporates behavioral data, including patient preferences and health literacy. Finally, contextual data—often referred to as social determinants of health (SDH)—accounts for living situations, stress levels, and economic constraints. Understanding these layers is the only way to move from generic care to precision medicine.
In a seminal paper published in The American Journal of Managed Care, researchers introduced the concept of the "sociobehavioral phenotype" to bridge the gap between clinical data and real-world outcomes. The study argues that just as oncologists look for "driver mutations" to select a targeted drug, healthtech systems must identify "driver socioeconomic risk factors"—such as housing instability or food insecurity—that are equally critical to the success of precision medicine and targeted therapy.
The technology infrastructure of personalization
To transition from generic care to personalized care plans, providers need a robust technical foundation. Personalization in healthtech is a competitive advantage for those who can integrate data across the entire healthcare delivery system. This infrastructure must support high-volume data processing while maintaining strict privacy standards.
The AI-HOPE-PM platform demonstrates that Large Language Models (LLMs) and Retrieval-Augmented Generation (RAG) can successfully automate the integration of fragmented clinical, genomic, and social data into a unified, searchable framework.
Data aggregation and member 360
Healthcare personalization starts with breaking down data silos. A member 360 view integrates information from electronic health records (EHR), patient portals, and wearable devices. This creates a holistic view of the medical history and the current status of the individual.
When a provider has a complete picture of the patient journey, they can anticipate needs rather than reacting to crises. Without this centralized data, care coordination remains fragmented. The technology infrastructure must act as a bridge between the clinical setting and the patient's daily life.
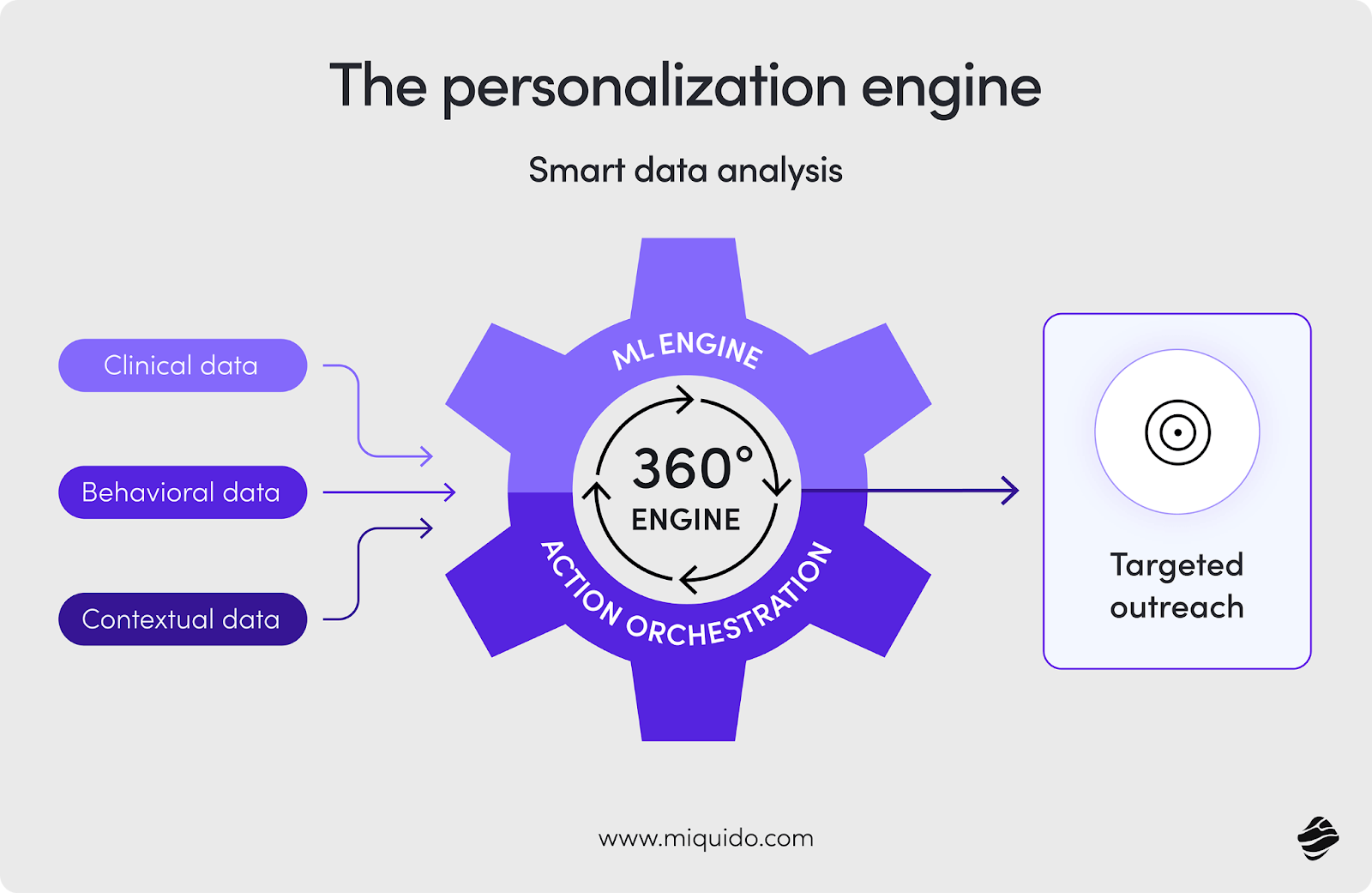
The personalization engine and action orchestration
Modern healthcare technology uses targeting based on machine learning to analyze health data analytics. A personalization engine acts on this data through action orchestration. For example, the system can trigger a personalized outreach message to a patient with diabetes who has not logged glucose levels in 48 hours.
This moves the interaction from a passive record to an active intervention. These personalized healthcare solutions ensure that the right message reaches the right person at the right time. By automating these touchpoints, healthcare providers can scale their impact without losing the human touch.
Remote patient monitoring and early detection
Through remote patient monitoring (RPM), providers receive real-time patient data. These patient monitoring tools allow for the early detection of complications. This shifts the focus of the healthcare ecosystem toward preventive care and disease prevention.
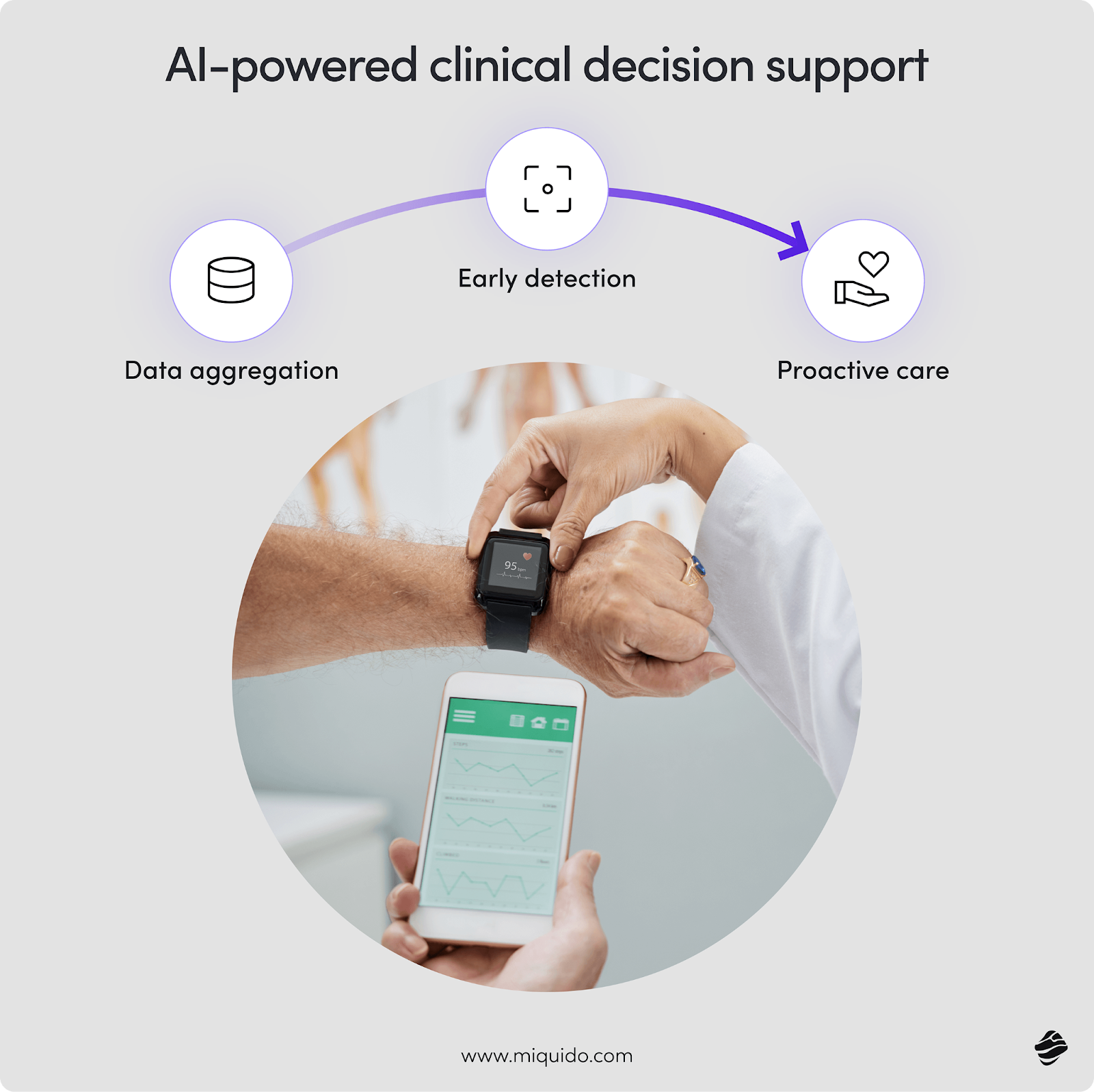
RPM is particularly effective in chronic disease management. Constant health monitoring allows for subtle adjustments to treatment plans before a patient requires hospitalization. This proactive approach improves clinical outcomes and significantly reduces healthcare costs over time.
Redefining the patient experience
The patient experience is largely about managing cognitive load. When a person is in a hospital or dealing with a chronic illness, their ability to process complex information is limited by stress. Designing a personalized patient experience means thinking about the entire journey: how they arrive, what they do, and how they leave.

We cannot design just one thing; we must always think about how a person gets there, what they do, and how they leave. In healthcare, it’s not just the hospital context—it’s the context of their emotional state, their stress, their limited cognitive abilities, and the worry that they had to take time off work just to be there.
Agata Rączewska, CX Expert
Personalized patient engagement
Effective patient engagement involves more than just sending reminders. It requires personalized recommendations delivered through digital health tools and virtual health assistants that provide 24/7 support. Digital personalization ensures that a patient feels seen and supported, even outside the clinic walls.
Health risk assessments (HRA) should lead directly to personalized wellness plans that the patient can actually follow. If a wellness plan does not account for a patient's economic constraints or health literacy, it is destined to fail. Personalization of healthcare must be as much about empathy as it is about algorithms.
In a comprehensive workshop report by the National Academies of Sciences, Engineering, and Medicine, experts established that health literacy is not a fixed trait but a "dynamic state"—a fluctuating capacity influenced by a patient’s immediate environment, stress levels, and the complexity of the medical system. This research highlights that even highly educated individuals can experience limited literacy when faced with the "cognitive load" of a diagnosis, creating a primary barrier to their engagement with electronic health records (EHRs) and their ability to act upon complex genomic risk data.
Case study: the fast oncology track
In Poland, the "Fast Oncology Track" is a prime example of care coordination and value-based care. By removing bureaucratic hurdles and focusing on treatment outcomes, the system reduces the time from diagnosis to surgery to just weeks.
This model treats the patient journey as a single, urgent workflow. It prioritizes the consumer experience by providing a clear path forward during a time of extreme vulnerability. The result is higher patient satisfaction and improved patient outcomes. This case study demonstrates that when the system is designed around the human, the medical results follow.
The business case for personalized care
While many healthcare organizations focus on short-term gains, the real value lies in long-term patient activation and loyalty.
Loyalization and LTV
By providing a personalized patient experience, clinics increase the lifetime value (LTV) of a patient. If a provider owns the care management and planning process, the patient is less likely to switch to a competitor. Personalization in healthtech becomes a tool for retention.
Cost efficiency and prevention
Chronic care management is expensive. Personalized interventions that improve medication adherence prevent costly emergency room visits. By investing in preventive care, organizations reduce the overall burden on the healthcare delivery system.
Quality of care
Tailored treatment plans lead to better clinical outcomes. When patients follow a personalized treatment path that fits their lifestyle, their recovery is faster and more sustainable.
Barriers to personalization in healthtech
Several hurdles still prevent the widespread adoption of personalized healthcare services. Legacy systems often do not communicate with each other, leaving healthcare data stuck in different departments. This "silo" mentality means that diagnostics, surgery, and recovery often operate as independent gardens.
Furthermore, healthcare requires more rigorous experimentation and measurement than other industries. Unlike e-commerce, where a failed A/B test has little consequence, a personalized treatment plan must be safe. This requires a strong foundation in bioinformatics and genetic testing to ensure that every recommendation is backed by science.
The role of precision medicine and genomics
The integration of genomics into daily clinical practice is a cornerstone of personalized care. Genetic testing allows doctors to prescribe medications based on a patient's specific genetic profile. This reduces the "trial and error" approach to medicine, particularly in behavioral health and oncology.
Personalized medicine uses these genetic insights to create highly specific personalized healthcare solutions. As genetic testing becomes more affordable, it will become a standard part of annual wellness visits. This level of detail allows for a degree of early detection that was previously impossible.
Social determinants of health and contextual care
Personalization must account for the world outside the hospital. Social determinants of health—such as housing stability, food security, and transport access—impact health outcomes more than clinical care alone.
A personalized care plan that ignores these factors is incomplete. For instance, prescribing a medication that requires refrigeration to a patient with unstable housing is a failure of care coordination. Digital health apps must begin to integrate these contextual data points to provide truly personalized interventions.
The future of personalized healthcare solutions
The future of personalized care is not just about drawing squares on a screen or improving a UI. It is about precision medicine fueled by genomics, supported by an empathetic consumer experience. As we move toward a more digital personalization model, the winners in the healthtech space will be those who use healthcare technology to simplify the patient's life.
Reducing frustration and providing a personalized treatment path makes healthcare feel human again. By focusing on health outcomes and the quality of care, organizations can build a system that supports the patient at every step of their journey. Personalized health care is no longer a luxury; it is the new standard for an efficient, effective, and empathetic healthcare ecosystem.
Miquido as a strategic partner in healthtech innovation
Successful personalization in healthcare requires more than just advanced software. It demands a partner who understands the intersection of medical compliance, user psychology, and scalable technology. Miquido has established itself as a strategic technological partner for the healthtech sector by focusing on these intersections.
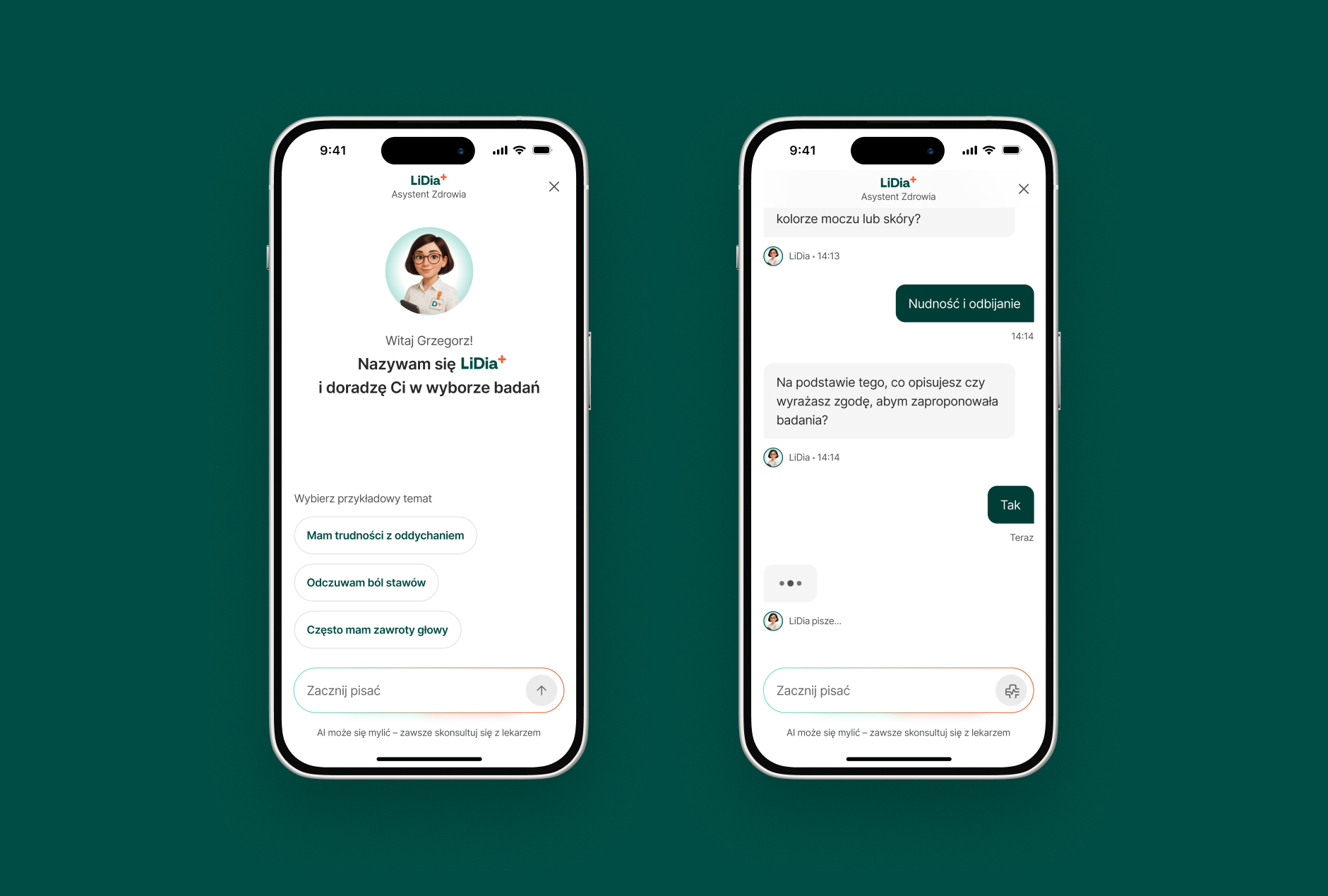
A primary example of this partnership is the transformation of Diagnostyka, Poland’s largest laboratory network. The challenge was to rebuild their digital presence into a platform that actively supports preventive healthcare. You can read the full details of this transformation in our Diagnostyka 2.0 case study.




![[header] healthcare trends 2026 – a patient centric future](https://www.miquido.com/wp-content/uploads/2023/12/header-healthcare-trends-2026-–-a-patient-centric-future-432x288.jpg)
![[header] how technology can improve patient experience a practical guide for healthcare providers](https://www.miquido.com/wp-content/uploads/2026/03/header-how-technology-can-improve-patient-experience_-a-practical-guide-for-healthcare-providers-432x288.jpg)
