Technology has enabled us to leap over many physical barriers, making remote healthcare possible and widespread. Its development now allows for surgeries to be performed in an automated and minimally invasive manner thanks to advanced precision medicine, transplanting artificial organs, or providing neurological stimulation.
And yet, many processes in the healthcare industry still hinder diagnosis or treatment and do not fully exploit the potential offered by telemedicine, interconnected medical devices, fast 5G networks and easily accessible AI.
Digital healthcare 4.0, with its interconnectivity, is meant to fill this gap. Its pillars are similar to those of industry 4.0, based on the free flow of data and big data analytics in real time. Medical 4.0, however, is a much more delicate matter, because at its center is – or at least should be – the human being and patient outcomes.
We will look at how, in practice, healthcare 4.0 technologies are created that actually make a difference.
Was the pandemic the "moment zero" for scaling Healthcare 4.0?
Do you remember the world before the pandemic? Think back to how healthcare functioned then. Teleconsultations were a futuristic rarity, and booking an appointment or solving a basic medical query via a chatbot – rather than languishing on a hold line for forty minutes – was almost unheard of.
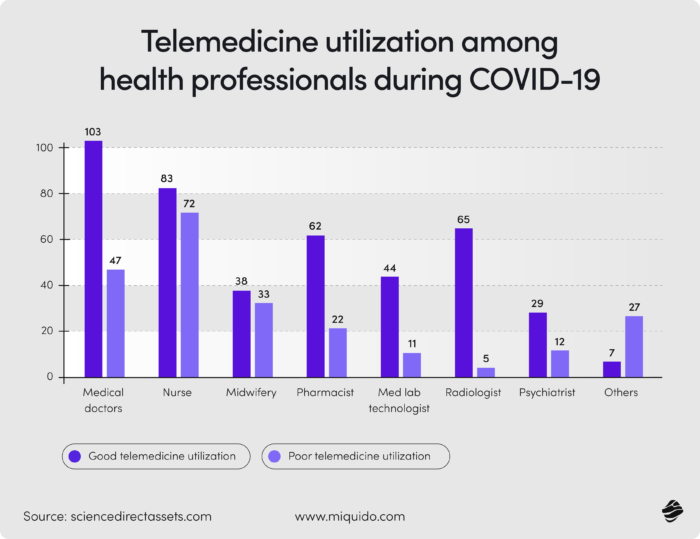
When the crisis hit, healthcare went remote, but that didn't automatically mean it became connected. While technology theoretically bridged the gap created by social distancing, it simultaneously birthed new frustrations. Patients attempted to navigate care digitally, only to be thwarted by poor system performance or rigid interfaces. Systems crashed, digital forms led to dead ends, and users were often left helpless with no physical alternative.
The pandemic exposed a systemic void: a lack of interoperability. Data didn't flow between facilities, documentation vanished into digital silos, and in the middle of this technical chaos, the patient was lost. This is precisely what Healthcare 4.0 aims to fix – a more integrated ecosystem where data moves securely between clinics, where wearables integrate with medical records for prevention rather than reaction, and where the patient is finally the focal point.
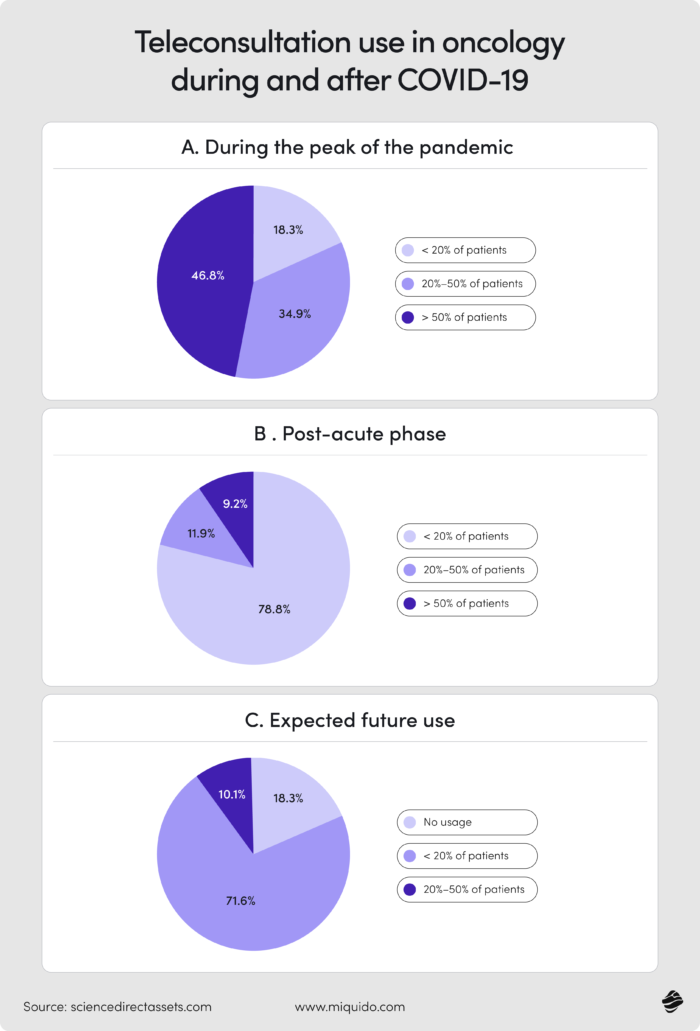
What is Healthcare 4.0 and why must the patient remain at its core?
Healthcare 4.0 is more than just interconnected tools or AI-assisted procedures; it is a "cyber-physical" ecosystem where human beings remain the priority. Even the most sophisticated automation cannot fix an inefficient process; in fact, poor tech often amplifies stress for both healthcare professionals and patients.
By prioritizing smart care solutions, we can bridge this empathy gap, ensuring that technology supports rather than complicates the delivery of medicine within modern healthcare systems.
Imagine a patient with an autoimmune condition who frequently relocates for work. In the current fragmented system, every move means a "blank slate" start. They must manually transfer thick folders of history and often repeat failed "step-therapy" treatments just to unlock advanced biologics in a new region.
In a Healthcare 4.0 model, their longitudinal health timeline follows them through integrated mobile health platforms. A new specialist can see five years of treatment efficacy and biostatistical trends in one click. Furthermore, remote patient monitoring allows for continuous oversight during the transition, bypassing months of administrative delay and physical suffering while significantly enhancing patient safety.
Case 2: The "parenthood burden" and multi-specialty coordination
Now think about a family with two small children, one of whom has complex allergies and neurological concerns. The parents currently act as "information couriers," chasing certificates and coordinating between specialists.
In a smart ecosystem, their healthcare app acts as a proactive concierge. It automatically flags upcoming necessary exams, syncs neurologist notes with the pediatrician, and provides digital-first certificates for schools. This returns agency to the parents, shifting them from "case managers" back to "caregivers" and allowing healthcare professionals to focus on clinical outcomes rather than paperwork.

How to design Healthcare 4.0 interfaces that heal instead of frustrating clinicians?
In high-stress medical environments, a poorly designed interface is more than an inconvenience – it is a clinical risk. User Experience (UX) in healthcare technology must account for the patient’s emotional vulnerability and the physician’s extreme cognitive load.
By moving toward a model of personalized medicine, developers can create AI-adjusted interfaces and dashboards that prioritize what really matters. These systems are designed to filter out visual and informational noise that would otherwise augment stress, ensuring that the most critical data points are always front and center.
The data deluge: Why usability is a clinical standard
An ICU physician faces an staggering 32,120 data points per shift. When Healthcare 4.0 tools are designed poorly, they contribute directly to physician burnout and measurable medical errors. Research from the Mayo Clinic Proceedings highlights a clear dose-response relationship: a mere 1-point improvement in system usability correlates with a 3% drop in burnout risk.
To combat this, modern healthcare applications must move beyond simple data entry toward connected care models that synthesize information into actionable insights rather than raw numbers.
Expanding the "healing" interface: AR and VR
The "interface" of Healthcare 4.0 is no longer limited to a flat screen. The integration of augmented reality (AR) allows clinicians to overlay digital diagnostics onto the physical world, reducing the need to look away from the patient to check a monitor.
Furthermore, virtual reality (VR) is proving to be a transformative tool in the "healing" ecosystem. While primarily used for educational purposes and empathy training for staff, VR is a cornerstone of neurological recovery (such as post-stroke rehabilitation or conditions like cerebral palsy).
Beyond clinical use, VR helps patients better understand their own conditions or test results by transforming abstract data into immersive, 3D visualizations. This high-fidelity interaction reduces the "fear of the unknown," turning a confusing diagnosis into a manageable roadmap for recovery.
The ROI of empathy: Impact on processes and finance
Pro-patient and pro-doctor design has a massive impact on a facility’s bottom line. When a healthcare 4.0 system reduces "information stress" – for example, by visualizing test results instead of presenting a "data wall" – patients are less likely to call the clinic in a panic, and doctors spend less time clicking and more time diagnosing.
- For the patient: Visualization reduces cognitive load and anxiety.
- For the clinic: Streamlined workflows increase throughput and reduce the "anonymity tax" of redundant testing.
Can Healthcare 4.0 build long-term loyalty through proactive well-being?
The traditional healthcare model has always been reactive: we wait for the pain, and then we seek the cure. Healthcare 4.0 flips this script. By shifting the focus from treating illness to maintaining wellness, providers can move from a transactional relationship to a subscription-like loyalty model based on continuous care and trust.
The data goldmine: From fitness tracking to clinical insight
Monitoring health through mobile applications and artificial intelligence, often integrated with wearable devices, is becoming a global standard. The user bases of Apple Health, Google Fit, and other ecosystems are ballooning, and their initial focus on "fitness and steps" is rapidly expanding into comprehensive medical data with the help of cloud computing and the internet of health things.
Think of the wealth of clinical evidence hidden in our smartphones. When integrated with diagnostic apps, hospital portals, or national patient accounts (like the Polish IKP), this data can seamlessly and securely – with patient authorization – support diagnosis and preventive practices. This "everyday scanning" of vitals like sleep patterns, menstrual cycles, or metabolic fluctuations allows systems to adjust treatment plans and schedule analysis automatically.
Such system could even notice a subtle, persistent shift in your resting heart rate or a drop in heart rate variability (HRV) before you even feel a symptom, triggering a proactive alert that prevents a cardiac event before it occurs.

Proactivity as a competitive edge: The "Diagnostyka" model
Proactive care is a win-win for the entire ecosystem: the patient avoids the "information stress" of self-monitoring, and the provider secures a loyal, healthier patient base. We see this in practice with the Diagnostyka app, which flags missing or overdue exams. The user doesn’t have to stay stressed, manually searching for what needs to be repeated – the system takes ownership of the timeline.
This level of "Path-Based Ownership" is where the most significant medical and financial outcomes are hidden. When a system removes the cognitive load from the patient, it stops being a utility and starts being a partner.
Ultimately, Healthcare 4.0 is about moving from a system that records illness to one that actively preserves safety. As the Silver Economy grows and global mobility increases, the providers who offer "Adaptive Accessibility" and proactive well-being will be the ones who define the new clinical standard.
Is legacy infrastructure the single greatest risk to Healthcare 4.0 ROI?
While we dream of AI-driven diagnostics and seamless data flow, many healthcare providers are building these "castles in the sky" on foundations of sand. The shift to Healthcare 4.0 is frequently stalled by the invisible barrier: legacy infrastructure.
The cost of technical debt: From breaches to bottlenecks
Delloite’s data shows a staggering reality – 60% of healthcare organizations still rely on outdated, fragmented systems. This isn't just a matter of slow interfaces, turning into critical security and financial liability. In 2025 alone, "technical debt" and unpatched legacy vulnerabilities contributed to massive data breaches affecting over 170 million medical records.
When a system is built on siloed, 15-year-old architecture, it cannot support the real-time interoperability required for Healthcare 4.0. You cannot run a smart treatment map if the underlying database takes three minutes to load a single PDF. For the provider, this inefficiency translates to lost time, increased risk of litigation, and a total ceiling on ROI.
The ethical dilemma: Zero-disruption modernization
Modernizing healthcare isn't like updating a retail app; you cannot simply turn the system off for maintenance. This creates a high-stakes ethical dilemma where zero-disruption modernization is now a prerequisite. We must ensure that the transition to AI and interoperability doesn't leave the most vulnerable behind.
The "small data" challenge
While AI thrives on big data, the ethical frontier of Healthcare 4.0 lies in "small data" – managing rare diseases where patient populations are limited and electronic health records are notoriously incompatible.
Unifying these fragmented records through advanced data analytics is an ethical imperative; without it, patients with rare conditions remain invisible to the very algorithms meant to save them. By leveraging edge computing, we can process this sensitive information closer to the source, ensuring that even localized or sparse data sets contribute to life-saving insights without compromising security.
Health equity and the digital divide
As we navigate this digital transformation, we face the risk that Healthcare 4.0 could widen the gap between the "digital haves" and "have-nots." If predictive analytics and life-saving proactive alerts are only available to those with the latest $1,000 wearable, we haven't revolutionized healthcare – we’ve merely digitized privilege.
True innovation must be inclusive by design, ensuring that "Adaptive Accessibility" extends to low-income populations and the "Silver Economy," turning technology into a tool for equity rather than exclusion.
How much does fragmentation cost, and can UX save the budget?
Fragmentation is often a multi-billion dollar leak in the global healthcare bucket. When the patient journey is broken, the financial consequences are immediate and severe.
The no-show crisis: A symptom of poor last-mile UX
Patient "no-shows" are a global epidemic, costing the healthcare industry an estimated $150 billion annually. While it’s easy to blame patient forgetfulness, this is often a symptom of poor "last-mile" UX. If a patient has to navigate a confusing phone tree or a legacy portal just to cancel or reschedule, they simply won't do it.
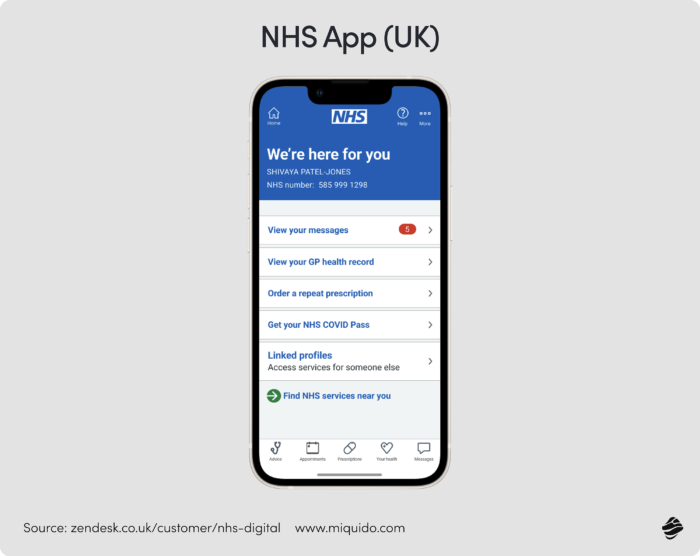
As seen with the NHS App in the UK, providing a centralized national platform where patients can book, cancel, or manage referrals in two clicks directly combats this waste. By returning agency to the patient through intuitive self-service, the system doesn't just improve satisfaction, but also protects its own resources.
Operational gains: Returning time to the doctor-patient relationship
Administrative waste currently accounts for 7.5%–15% of total healthcare spending. Online Appointment Scheduling (OAS) and automated triage are the "low-hanging fruit" of Healthcare 4.0 that offer the fastest ROI.
- Reducing "blank slate" waste: When UX allows for pre-visit data collection and automated history summaries, the doctor doesn't spend the first 10 minutes of a 15-minute appointment typing.
- Streamlining the path: Efficient UX reduces the cognitive load on administrative staff, allowing them to focus on complex cases rather than routine scheduling.
By fixing the "friction of the journey," healthcare providers can transform their budget from one that subsidizes its own inefficiency into one that invests in better clinical outcomes. Good CX is, ultimately, the most effective cost-optimization strategy available in 2026.
Achieving excellence in digital health
Putting the patient first is a strategic advantage that makes high-quality customer experience in healthcare both possible and highly profitable. Embracing the imperative to improve patient experience allows us to create digital health solutions that truly make a difference while maximizing healthcare quality.
Our proven track record with smart and connected health leaders like Diagnostyka, InVision, Pando and Ventricle shows that investing in user-centric care pays off in both loyalty and outcomes. Leveraging our deep expertise in healthcare and wellness apps, we are ready to help you turn this patient-first vision into a market-leading reality.

![[header] healthcare 4.0 an ultimate guide. how technology is redefining care, life, and human connection](https://www.miquido.com/wp-content/uploads/2026/03/header-healthcare-4.0_-an-ultimate-guide.-how-technology-is-redefining-care-life-and-human-connection.jpg)

![[header] healthcare 4.0 an ultimate guide. how technology is redefining care, life, and human connection](https://www.miquido.com/wp-content/uploads/2026/03/header-healthcare-4.0_-an-ultimate-guide.-how-technology-is-redefining-care-life-and-human-connection-432x288.jpg)


![[header] healthcare trends 2026 – a patient centric future](https://www.miquido.com/wp-content/uploads/2023/12/header-healthcare-trends-2026-–-a-patient-centric-future-432x288.jpg)